Human breast milk (HBM) is the most ideal and complete form of nutrition for an infant. Its composition changes throughout lactation, consistent with the changing needs of the infant. For this reason, the World Health Organization (WHO) and the American Academy of Pediatrics (AAP) both recommend exclusive breastfeeding for six months, followed by continued breastfeeding in conjunction with complementary feeding up to 2 years of age or longer, as desired by the mother and infant.
Potential uses for breast milk beyond consumption include shortening the cord stump separation time, and improving certain conditions like dry eye syndrome, atopic eczema, diaper dermatitis, and other diseases. In the same manner, breastfeeding has positive effects not only on the feeding baby, but for the mother offering her breast milk as well.
Benefits of Breast Milk and Breastfeeding
For the Infant
HBM is able to provide the complete nutrition, as well as many bioactive health factors, for a newborn infant. Aside from fundamental nutrients present in breast milk, it is also a source of commensal bacteria that enhance infant health by preventing adhesion of pathogens and promoting gut colonization of beneficial microbes.
Therefore, breastfeeding has been linked to less incidence of gastrointestinal (GI) disease, such as GI infections, diarrhea, and necrotizing enterocolitis. This, in turn, led to decreased mortality rates among breastfed infants compared to formula-fed babies.
Studies have also reported that breastfed infants have decreased risk of chronic diseases like irritable bowel syndrome and Crohn’s disease both in childhood and adult life. In addition, prolonged breastfeeding has been associated with improved cognitive development among infants (Lyons et al., 2020).
Other benefits of breast milk for the infant include the following: decreased incidence of respiratory and urinary tract infections, and otitis media, as well as reduced risk of asthma, allergy, and types I and II diabetes mellitus. Moreover, it was found to have protective effects against the development of non-communicable diseases like obesity and cardiovascular disease (Zhu & Dingess, 2019).
For the Mother
Breastfeeding burns extra calories and can help mothers lose their pregnancy weight faster. The hormone oxytocin, which is released through breastfeeding, helps the uterus contract and return to its pre-pregnancy size, which also reduces uterine bleeding after birth.
Zhu & Dingess (2019) stated that the act of breastfeeding has also shown other benefits for the mother’s health. This includes decreased risk for development of rheumatoid arthritis, cardiovascular disease, diabetes mellitus, and breast and ovarian cancers.
Breastfed babies cry less overall, and they have fewer incidences of childhood illnesses. Breast milk is always clean and has the right temperature, so there is no need for additional preparations prior to feeding. These result in increased calmness and satisfaction for the mother and the whole family.
In addition, the act of breastfeeding produces naturally soothing hormones (oxytocin and prolactin) that promote positive feelings and reduce stress in the mothers. Other emotional benefits of breastfeeding include: increased maternal confidence and self-esteem, improved physical and emotional bonding between the mother and her child, and improved ability of the mothers to read their infant’s cues that would shape their baby’s trust.
Other Uses for Breast Milk
Cord Separation
In some societies of Kenya and some areas of Turkey, breast milk is one of the methods used for caring for the umbilical cord stump of the newborn. It is known that HBM is a source of transforming growth factors alpha and beta (TGF-A and TGF-B) and the insulin-like growth factors 1 and 2 (IGF-1 and IGF-2), which promote muscle and cartilage repair and wound healing. Meanwhile, the WHO recommendation is for chlorhexidine to be used as an antiseptic for the cord when needed (Abbaszadeh et al., 2016).
Abbaszadeh et al. did a research in 2016 to compare the effect of HBM and chlorhexidine on cord separation among newborns in Iran. Their results showed a significant difference between the group who used breast milk on the cord stump and the other group who used chlorhexidine, in terms of mean cord separation time. The HBM group had shorter (5-9 days) cord separation time compared to the chlorhexidine group (6-20 days).
Shorter cord stump separation also means reduced risk of infection on the umbilical site, which may lead to neonatal infections like omphalitis and sepsis. Therefore, topical use of breast milk on the umbilical cord can be a cheap, easy and effective method for umbilical cord care. Still, further studies are needed to verify this conclusion.
Dry Eye Syndrome
At a tertiary eye center in South India, HBM was noted to be the most commonly used traditional eye medicine (TEM) for the treatment of corneal ulcers. Breast milk contains components that have been studied in the treatment of dry eye syndrome (DES), including epithelial growth factor (EGF), vitamin A, lactoferrin, oligosaccharides, and omega-3 and omega-6 fatty acids. HBM likewise contains components that protect against infection, such as lysozymes, immunoglobulin A (IgA), immunoglobulin G (IgG), cytokines like interleukin (IL)-10, and β-defensin-2 (Diego et al., 2016).
To demonstrate the efficacy of breast milk in the treatment of DES, Diego et al. in 2016 used the BAK (benzalkonium chloride)-induced dry eye mouse model. To induce DES in mice, BAK (0.2%) was applied to the mouse ocular surface. Afterward, the mice were administered with cyclosporine, a standard therapy for this condition, or HBM. Therapeutic efficacy was compared and determined by histological measurements of corneal epithelial thickness.
Results revealed that administration of HBM prevented the reduction in corneal epithelial thickness, similar to the outcomes seen on mice treated with cyclosporine. Hence, the topical application of breast milk provides prevention of DES and has a potential to be an effective treatment in humans, especially for patients with limited health care access or those more inclined to TEM (Diego et al., 2016). However, further studies are needed to determine the safety of the use of breast milk for treatment of DES in humans.
Atopic Eczema
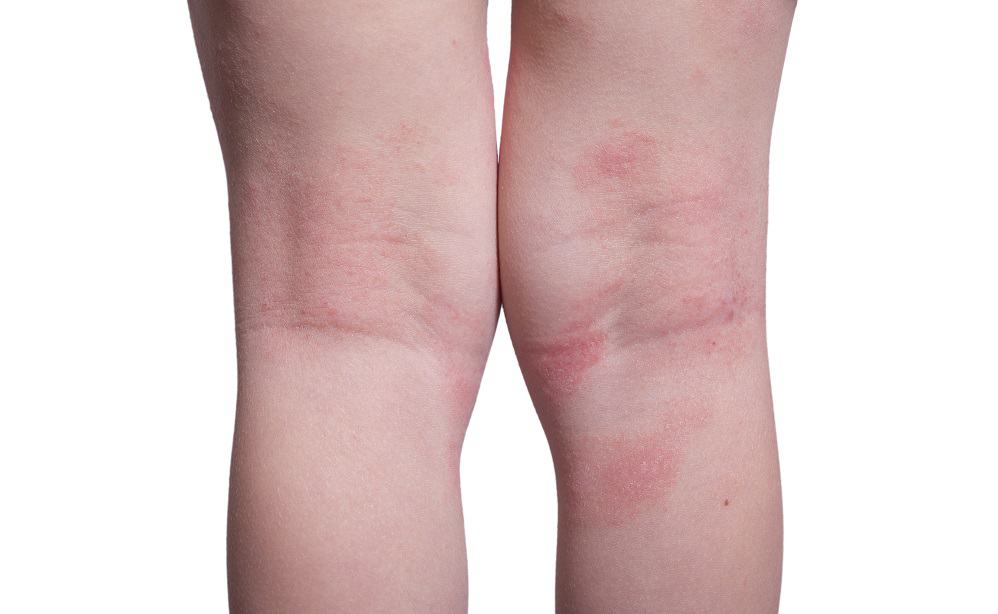
Atopic eczema is a chronic, pruritic, relapsing skin disease. Its pathogenesis involves the interplay between barrier dysfunction, genetic, immunological and environmental factors, and colonization by Staphylococcus aureus (S. aureus). First line treatment targets the barrier dysfunction by providing optimal skin care through emollients and baths, while inflammation is managed with topical corticosteroids.
HBM contains immune components, including antimicrobial and anti-inflammatory factors, which could potentially have an effect on eczematous skin. A pilot study was done by Berents et al. (2015) to assess the effects of application of breast milk to eczema spots in children. Only six patients were able to complete the study. However, results showed that topical administration of HBM had no effect on eczema spots.
Read More: The Benefits of Breast Milk Baths for Babies
In contrast, Kasrae et al. in 2015 randomized 104 Iranian infants with atopic dermatitis for 21 days of treatment with either 1% hydrocortisone or breast milk. The percentage of healed infants was statistically same with 81.5% in the HBM group and 76% in the hydrocortisone group. Their findings suggest that breast milk can improve atopic eczema with similar results as 1% hydrocortisone ointment, but without the side effects and cost.
Diaper Dermatitis
Diaper dermatitis is a common dermatological disease during infancy, which occurs due to the combined effect of irritants (diaper), urine, and stool. It is characterized by an inflammatory eruption of the skin in the diaper area. Also called diaper rash, it can cause pain and stress for both infant and caregivers.
Breast milk contains antibodies that could potentially treat minor illnesses. Hence, Seifi et al. in 2017 studied the effect of topical administration of breast milk on diaper dermatitis in Iran. 30 infants between the ages of 0 and 12 months who had diaper rash participated in the study. Results showed a significant difference between the case and control groups, in terms of the number of rashes and lesion score, most notably on the fifth day.
Likewise, the effects of topical application of HBM and 1% hydrocortisone were also compared in the treatment of diaper dermatitis. The study consisted of 141 infants aged 0 to 24 months. The hydrocortisone group was instructed to apply the medication twice a day for seven days, while the mothers in the breast milk group were asked to rub their milk on the infant’s affected area at the end of each breastfeeding session. The presence of diaper rash was checked daily using a six-point scale, and in both groups, improvement was statistically similar. The authors concluded that breast milk was as effective and safe as hydrocortisone 1% ointment in the treatment of diaper dermatitis (Farahani et al., 2013).
Reports on Other Diseases
It is said that topical HBM is one of the traditional medicines used for various injuries, ulcers, and infections for decades. Amiri-Farahani et al. (2020) selected and reviewed 20 articles from 1990 to 2018 to study the effects of breast milk when applied topically on dermal and optical diseases. They concluded that the use of breast milk appears to be an effective and safe alternative treatment to a number of skin conditions, including atopic dermatitis, diaper dermatitis, conjunctivitis, scratches, insect bite, perineal ulcer, and nipple ulcer.
Breast milk contains anti-inflammatory and antioxidant properties, such as vitamins A, C and E, catalase, glutathione peroxidase, prostaglandins, platelet activators, and leukocytes. These components may be the potential underlying cause for the curative effects of breast milk. However, more research is needed to reach a definitive conclusion as to the efficacy and safety of topical use of HBM in similar or different injuries among different populations.
In contrast, Gungor et al. in 2019 reported that after a systematic review of articles that have been published between January 1980 and March 2016, they concluded that evidence of breast milk’s effects on food allergies, allergic rhinitis and atopic dermatitis is limited. Hence, more research is needed to be able to formulate definitive recommendations.
Final Thoughts
A vast number of data is available to prove the benefits of breast milk when consumed orally by an infant. However, researches conducted for other uses of breast milk (particularly when applied topically on the skin) remain to be limited. There are conflicting results seen among published studies about this topic.
Nevertheless, the human breast milk is a good, natural, and massive source of nutrients, good bacteria, anti-inflammatory and antimicrobial factors. It has a huge potential to be used other than for consumption.
Though potentially useful and effective, specific guidelines need to be formulated regarding the use of breast milk as treatment for certain skin conditions. Until the above-mentioned uses for breast milk become scientifically established, make sure to consult your physician before trying out the use of HBM as a home remedy.
References
- https://my.clevelandclinic.org/
- https://www.webmd.com/
- Abbaszadeh, F., Hajizadeh, Z., & Jahangiri, M. (2016). Comparing the impact of topical application of human milk and chlorhexidine on cord separation time in newborns. Pakistan Journal of Medical Sciences 32(1), 239-243. doi: 10.12669/pjms.321.8223
- Amiri-Farahani, L., Sharifi-Heris, Z., & Mojab, F. (2020). The anti-inflammatory properties of the topical application of human milk in dermal and optical diseases. Evidence-Based Complementary and Alternative Medicine 2020. https://doi.org/10.1155/2020/4578153
- Berents, T. L., Ronnevig, J., Soyland, E., Gaustad, P., Nylander, G., & Loland, B. F. (2015). Topical treatment with fresh human milk versus emollient on atopic eczema spots in young children: A small, randomized, split body, controlled, blinded pilot study. BMC Dermatology 15, 7. doi: 10.1186/s12895-015-0027-9
- Diego, J., Bidikov, L., Pedler, M., Kennedy, J., Quiroz-Mercado, H., Gregory, D., Petrash, J. M., & McCourt, E. (2016). Effect of human milk as a treatment for dry eye syndrome in a mouse model. Molecular Vision 22, 1095-1102.
- Farahani, L. A., Ghobadzadeh, M., & Yousefi, P. (2013). Comparison of the effect of human milk and topical hydrocortisone 1% on diaper dermatitis. Pediatric Dermatology 30(6), 725-729. doi: 10.1111/pde.12118
- Gungor, D., Nadaud, P., LaPergola, C., Dreibelbis, C., Wong, Y. P., Terry, N., Abrams, S., Beker, L., Jacobovits, T., Järvinen, K., Nommsen-Rivers, L., O’Brien, K., Oken, E., Pérez,-Escamilla, R., Ziegler, E., & Spahn, J. (2019). Infant milk-feeding practices and food allergies, allergic rhinitis, atopic dermatitis, and asthma throughout the life span: A systematic review. American Journal of Clinical Nutrition 109(Suppl 1), 772-799. doi: 10.1093/ajcn/nqy283
- Kasrae, H., Farahani, L. A., Yousefi, P. (2015). Efficacy of topical application of human breast milk on atopic eczema healing among infants: A randomized clinical trial. International Journal of Dermatology 54(8), 966-971. doi: 10.1111/ijd.12764
- Lyons, K., Ryan, C. A., Dempsey, E., Ross, R. P., & Stanton, C. (2020). Breast milk, a source of beneficial microbes and associated benefits for infant health. Nutrients 12(4), 1039. https://doi.org/10.3390/nu12041039
- Seifi, B., Jalali, S., & Heidari, M. (2017). Assessment effect of breast milk on diaper dermatitis. Dermatology Reports 9(1), 7044. doi: 10.4081/dr.2017.7044
- Zhu, J., & Dingess, K. (2019). The functional power of the human milk proteome. Nutrients 11(8), 1834.




